MEDICAL FIELD
2024/06/21
[Dialysis Medical Care and SDGs #2] Treatment Options: What is Sustainable Dialysis Medical Care in the Future?
- Hemodialysis
- Interview
- Medicalbusiness
![[Dialysis Medical Care and SDGs #2] Treatment Options: What is Sustainable Dialysis Medical Care in the Future?](/media/kMxvJwAdHOfgot6LqeZcH0WkXH45Q5buehtbuYnK.jpg)
Index
Now that people are seeking to realize a sustainable society due to the adoption of the SDGs, what is required in the field of dialysis medical care?――In this series, we invited Dr. Ken Tsuchiya, Specially Appointed Professor at Tokyo Women's Medical University, to discuss sustainable dialysis medical care from the perspectives of both a healthcare professional and a manufacturer that develops medical devices.
In the first installment, we asked in detail about the environmental issues and workstyles surrounding dialysis medical care with respect to sustainability. In this second installment, we will ask about the issues regarding the options for dialysis treatment and the desired dialysis medical care in the future.
Ken Tsuchiya: M.D., PH.D., Specially Appointed Professor, Department of Blood Purification, Tokyo Women's Medical University. A leader in the fields of dialysis and kidney disease in Japan, serving as President of the 67th Annual Meeting of the Japanese Society for Dialysis Therapy. Nikkiso Co., Ltd. Satoshi Takeuchi: Chief manager of Equipment Development Department at the Medical Research and Technology Center of the Medical Division. *This article is an English translation of one originally published in Japanese on April 5, 2023. |
Dialysis Medical Care and Treatment Options
 Dr.Tsuchiya
Dr.Tsuchiya
Dr. Tsuchiya: In the second installment, I would like to discuss the essence of medical care linked to Goal 3. Good Health and Well-Being in the SDGs.
Hemodialysis is an important treatment to replace the function of kidneys that are damaged by disease, but it cannot completely compensate for the function of healthy kidneys. The treatment can only replace about 10% of this function in terms of removing toxins.
So, the patient needs to take large amount of medicines in addition to hemodialysis in order to adequately eliminate waste products and excess water accumulated in the body, which is the function the kidneys are originally responsible for. Furthermore, since the function of the kidneys is not perfect, various complications may occur, such as itching on the body, brittle bones, and accelerated arteriosclerosis, no matter how much effort the patient makes with respect to treatment and maintaining a regular life.
These burdens are already huge, but recently the age of patients who start dialysis treatment is increasing, and there are many patients who start dialysis in their 70s......It can be said that it is becoming more difficult for patients to continue with treatment, such as due to the nature of the treatment that requires hospital visits three times a week.
――At present, is there any way to address the issue of the burden on patients or any treatment alternatives to hemodialysis?
Dr. Tsuchiya: In addition to hemodialysis, there are some other options for renal replacement therapy to replace the function of the kidneys, such as peritoneal dialysis and kidney transplantation.
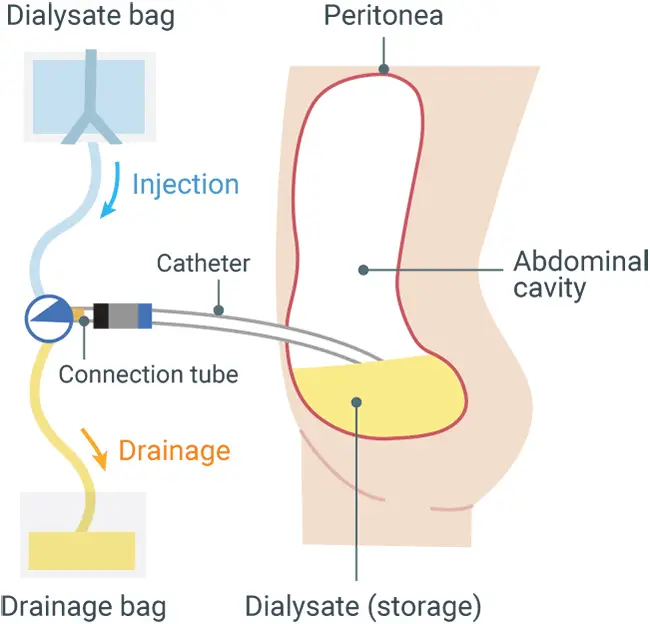
Peritoneal dialysis is a treatment to replace the function of the kidneys by placing dialysate in the abdomen and transferring waste products and excess water from the blood to the dialysate through a membrane that covers the internal organs (peritoneum). Its characteristics are that dialysis performed over 24 hours causes little change in blood pressure with less burden on the body, and that the treatment itself can be performed at home and the patient needs to visit the hospital only once a month.
Kidney transplantation, which recovers the function of the kidneys through a kidney transplant, can replace about 50% of the original function of the kidneys, thereby reducing the risk of complications compared with dialysis treatment. As long as the patient takes medicine that suppresses the immune response in the body, the patient will be able to live without restrictions and burdensome dialysis treatment for the time being.
――Despite these options, why do the vast majority of patients in Japan choose hemodialysis?
Dr. Tsuchiya: One major factor may be that hemodialysis has spread nationwide and become the least stressful treatment for patients because there are a wide range of hospitals to choose from, thanks to the efforts of the national government and healthcare professionals in order for patients to be able to receive dialysis treatment anywhere comfortably. In contrast, there are only a limited number of facilities and healthcare professionals that can provide kidney transplant surgery and peritoneal dialysis.
There may also be various other factors, such as the necessity of taking dialysate in and out by the patient himself/herself several times a day and the uncomfortable or oppressive feeling in putting dialysate in the abdomen in the case of peritoneal dialysis, and the reluctance about organ transplantation or donation and the lack of donors in the case of kidney transplantation.
Currently, as many as about 95% of patients choose hemodialysis as a renal replacement therapy, and there is a growing belief that this imbalance should be corrected as much as possible.
――Regarding the issue of treatment options explained by Dr. Tsuchiya, is there anything that Nikkiso is working on?

Maeda from Nikkiso: As the concept of shared decision making (SDM) spreads, we are working to provide information to create an opportunity for physicians to introduce various treatments to patients. Currently, we produce a booklet to introduce the options of renal replacement therapy, and it is actually being used by physicians.
Although it is very difficult for us to directly contribute to the expansion of treatment options, we want to continue such provision of information as one of roles that manufacturers can play.
Takeuchi from Nikkiso: In addition, we are continuing effort to reduce the burden on patients in order to reduce the risk of blood loss as much as possible and enhance the quality of life (QOL) during treatment by strengthening monitoring functions, such as equipping dialysis machines with a function to predict in advance a reduction in blood pressure, one of the most common problems during treatment.
We want to provide treatment that satisfies patients as it is protective medical care

――What initiatives and efforts are currently being made at medical sites to provide better dialysis medical care to patients?
Dr. Tsuchiya: First, in order to ensure that patients receive hemodialysis comfortably, we provide support for hospital visits and support for daily life such as eating methods and medication management in cooperation with dietitians and pharmacists.
In addition, while it had been common that men and women receive hemodialysis in the same room, today there are facilities that separate treatment spaces and floors for men and women so that they can relax as much as possible. The awareness of caring for patients' feelings and privacy is also increasing.
For the purpose of enabling the selection of treatment methods other than hemodialysis, the national government and healthcare professionals are working together to take measures.
In April 2020, for example, the Ministry of Health, Labour and Welfare revised medical fees to evaluate the active initiatives of facilities to carefully provide information on peritoneal dialysis and kidney transplantation, and surgery thereof. Against the backdrop of this revision and the spread of SDM, it is expected that patients will have a better understanding of each treatment method and be able to choose the one that suits them.
In the near future, conservative kidney management (CKM) is also expected to become a new option. This refers to palliative care provided to mitigate symptoms and distress when patients choose not to use renal replacement therapy or not to continue dialysis treatment.
In order to gain the understanding of a patient's family and society regarding this therapy, an attempt is currently ongoing to create guidelines on the criteria for starting CKM and the contents of palliative care.
――Aiming for the situation where the patients choose by themselves whether or not to undergo renal replacement therapy (kidney transplantation, peritoneal dialysis, hemodialysis) and which to choose if they undergo one?
Dr. Tsuchiya: Yes. Renal replacement therapy only complements the original function of the kidneys, which means, so to speak, protective medical care.
In particular, dialysis treatment does not seek to cure disease but to continue the same treatment. It is currently said that the function of the kidneys is maintained for about 20 years from kidney transplantation with a probability 60 to 70%, and dialysis treatment is required after that in many cases. This is the fate and difficulty of renal replacement therapy, but......I believe we should continue to provide patients with detailed information and have a dialogue with them so that they can make choices after they adequately understand each treatment method.
Healthcare professionals and manufacturers supporting innovation are inseparable

――What is the vision of Nikkiso as we aim for the sustainable dialysis medical care that has just been described?
Maeda from Nikkiso: First of all, as a manufacturer, we recognize that we must urgently address the current issues, such as the discovery and utilization of new materials that solve the issues of waste, in order to come as close to sustainable dialysis medical care as possible.
And above all, we will keep making efforts to continuously contribute to providing safe and secure hemodialysis treatment to patients. Specifically, we will increase the time available for healthcare professionals to interact with patients by continuously providing enhanced functions that achieve monitoring, automation and labor-saving, and support the operation of dialysis facilities by reducing utilities and other costs.
Takeuchi from Nikkiso: As the first step toward that goal, the theme we would like to consider is the utilization of AI. A large amount of patient data (treatment data, blood test results, etc.) is accumulated during treatment that takes four hours, three times a week. Utilizing this data, we aim to realize new ways of treatment so that, for example, the dialysis machine proposes dialysis conditions to the healthcare professionals, or the pump of the dialysis machine is automatically controlled to stabilize blood pressure before it falls.
――From the standpoint of a healthcare professional, is there anything you expect from Nikkiso, Dr. Tsuchiya?
Dr. Tsuchiya: Looking back at the history of hemodialysis treatment......the evolution of dialyzers and blood tubing lines enabled selective and efficient elimination of bad substances that accumulated in the body. The finding that water used for treatment must be clean, and the advancement of technology to achieve it, greatly reduced complications.
Manufacturers who have put their heart and soul into such innovation, and we as healthcare professionals, are truly inseparable, and I believe that current dialysis medical care would be impossible without the manufacturers. I hope they will continue such efforts together with us.

――Finally, please tell us about how dialysis medical care should be in the future, Dr. Tsuchiya.
Dr. Tsuchiya: Good medical care can only be achieved if the motivation and effort of healthcare professionals, the cooperation of patients, the development of medicines and medical devices, and the promotion by the national government all work in harmony.
No matter how much effort physicians and patients make, there are some things that cannot be done without a budget. So, in order to gain social consensus, we need to work hard to solve environmental and labor issues.
There is almost no other medical treatment like dialysis medical care that is performed with the participation of and together with patients. I believe that we should make every effort for SDM and reducing the burden of treatment so that patients are willing to cooperate.
――Thank you very much for valuable comments in the first and second installments.
Pickup
-
 MEDICAL FIELD
MEDICAL FIELD
Empowering Asia’s Expanding Dialysis Treatment with Nikkiso’s Advanced Technology and Comprehensive Support
- Hemodialysis
- Interview
- Medicalbusiness
2025/10/30
-
 MANUFACTURING
MANUFACTURING
Pumps also actively used in semiconductor manufacturing: 20 years of history of compact, high-speed canned motor pumps
- Technology
- Interview
- Pump
- Semiconductor
2025/05/21
-
 MANUFACTURING
MANUFACTURING
Nikkiso's DX initiatives: CAE Support Department continues to evolve, aiming to eliminate dependence on the skills and expertise of specific people
- Technology
- Interview
2025/04/09





